So what regulates how much drug can be absorbed by the GI tract?
- For starters the rate of dissolution of the pill, if taken in pill form.
- The surface area for absorption - for example the stomach's surface area is small and covered by a thick mucous layer, while the villi in the upper intestine give it a large surface area that's able to absorb a drug better.
- The pKa of the drug and its lipid solubility - Different areas in the GI tract have different pH, and you need to get the drugs through the membrane barriers into the blood plasma.
Controlled Release
The goal of this type of preparation is to produce slow, uniform absorption of the drug for 8 hours or longer. This is cool because the patient can take less pills (making it easy to comply with treatment), therapeutic effects can be maintained overnight, and you decrease the incidence of undesired effects because you avoid the peak of drug concentration the bloodstream that occurs when you use immediate-release dosage.
Of course not everything is unicorns and rainbows - there are several drawbacks. There is greater variability between patients on the systemic concentration of the drug. Another problem is that if the controlled release mechanism fails, and all the drug can be released at once. Since the amount of drug in the controlled release preparation is higher than the drug amount in immediate release preps, this "dose-dumping" can result in drug concentrations high enough to cause toxicity. Controlled release is best used with drugs that have a short half-life (<4>
Sublingual Administration
Your oral mucosa can also absorb drugs, especially if they are nonionic (has no positive or negative charges) and highly lipid soluble. Nitroglycerin is a perfect example:
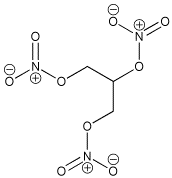 *Those plus and minus signs are partial charges, not formal charges, and arise from the electrons in those "tips" of the molecule liking the 2 Oxygens (O's) better than the Nitrogen (N's) and spending more time (in average) with the O than with the N.
*Those plus and minus signs are partial charges, not formal charges, and arise from the electrons in those "tips" of the molecule liking the 2 Oxygens (O's) better than the Nitrogen (N's) and spending more time (in average) with the O than with the N.Nitroglycerin also has various things going that makes it an awesome candidate for sublingual administration:
- It's very, very potent. You only need to absorb a few molecules of it for it to have a therapeutic effect.
- The mouth's veins drain into the superior vena cava, and thus goes straight to the heart, bypassing the hepatic first pass metabolism.
This is very useful when the patient is unconscious or is vomiting. About 50% of the drug absorbed through the rectum will bypass the liver and thus you loose less drug to first pass metabolism than with oral administration. On the down side, rectal absorption absorption can be irregular and incomplete, and lots of drugs can irritate the rectal mucosa.
*I have no idea how I resisted making many, many puns.
NEXT: On Pins and Needles: Parenteral injection


No comments:
Post a Comment